
The Femina Physical Therapy Blog
Featuring original articles by our staff about current events and trends
With emphasis on vaginismus, pregnancy and postpartum best practices, treatments for incontinence, and other topics related to the health of your pelvic floor.
Featured From the Blog:
Introducing The Origin Fund - Helping Women in Need

Helping Women in Need With Our Community in Mind
The Origin Fund is dedicated to facilitating access to services that address a person’s physical, emotional and medical needs. Our focus is on individuals with pelvic health dysfunctions, and we are dedicated to improving the biopsychosocial aspects of each person as a whole. Through education, outreach and providing access to these services, we can support individuals on their journey to address their pain and dysfunction—linking patients to our network of referrals that provide these services.
Therapeutic Breast Massage in Lactation (TBML)

Therapeutic Breast Massage in Lactation Can Help Make Breastfeeding Less Painful
Breastfeeding is widely accepted as the normal standard for providing nutrition to newborns, however, many women who do not reach their breastfeeding goals. US national data stated that breast pain was a commonly reported reason for women weaning less than 1 month postpartum. Within that segment, 29% of women who participated in the study stated that “breastfeeding was too painful” to continue.
In the same study, 24% of women reported “breasts feel(ing) too full or engorged” as another reason to discontinue breastfeeding prior to 1 month postpartum.1 Currently, The American Academy of Pediatrics recommends exclusive breastfeeding of infants for the first six months of life. As physical therapists who treat patients with postpartum conditions, we are well positioned to make a big impact on patients with breastfeeding related pain and reduce barriers to continued breastfeeding!
Treating Bloating and Abdominal Distension: a Multi-Disciplinary Team

Why a Multi-Disciplinary Team is Best for Treating Bloating and Abdominal Distension
Bloating, abdominal distension, loose stools, constipation, abdominal or pelvic pain, fatigue, brain fog, weakness, nutritional deficiencies… these symptoms may be caused by a variety of gastrointestinal or pelvic conditions. If you are experiencing any of these symptoms, this article is a good place to start when deciding who to have on your care team, and what treatments can help!
- Details
- Written by: Staff
- 5350 Views

What's the Link Between Endometriosis and Central Sensitization?
Endometriosis affects roughly about 10% of reproductive-age women, and is characterized by endometrial-like lesions that grow outside of the endometrium (the lining of the uterine wall). Women with endometriosis have symptoms such as: chronic pelvic pain, dysmenorrhea, abdominal pain, infertility, constipation, interstitial cystitis/painful bladder syndrome, and more.
Often endometriosis is treated through hormonal management and/or surgically. However, 18-27% of patients with endometriosis treated via hormonal medications reported no relief from symptoms. About 20% of patients with endometriosis treated through surgical excision or ablation continued to experience chronic pelvic pain and other endometriosis symptoms. Moreover, 70 to 80% of women with chronic pelvic pain with confirmed endometriosis lesions do not have lesions in the areas where they experience symptoms.
- Details
- Written by: Staff
- 3168 Views

What causes incontinence during pregnancy?
There are many causes for incontinence during pregnancy and postpartum. Some of the proposed factors are:
- hormonal changes,
- pelvic floor muscle and connective tissue modifications,
- bladder neck widening (due to the weight of both the uterus and the growing fetus),
- anatomical injuries during delivery.1, 2
A hormone called relaxin is produced during pregnancy to help soften the muscles and ligaments in preparation for delivery. As the uterus and baby grow throughout pregnancy more load is placed on the pelvic floor muscles causing the pelvic floor muscles to become weaker.3 Also constipation, which is commonly seen in pregnancy, puts an additional load on the pelvic floor.4 Furthermore, the pelvic floor has additional strain placed on it during labor; the pelvic floor muscle is stretched five times its original length.5
- Details
- Written by: Staff
- 5504 Views

What Are The Connections Between Endometriosis and Sleep?
March is Endometriosis Awareness Month.
The endometrium is the lining of the uterus. When there is tissue similar to the endometrial lining that is growing outside of the uterus, it is called endometriosis. Endometrial lesions can be on the ovaries, vaginal walls, bladder, colon, and more. Endometriosis affects up to 10% of the general population and can be quite debilitating as common symptoms include dysmenorrhea, dyspareunia (pain with sex), infertility, bloating, gastrointestinal symptoms, and chronic pelvic pain.
- Details
- Written by: Staff
- 4537 Views

Pelvic Floor Rehabilitation for Prolapse Surgeries
Including both Pre and Post Operative Situations
Suffering from symptoms of pelvic heaviness? Experiencing a feeling that there is a bulge down there or something is falling out of your vagina? Have trouble having a bowel movement or experiencing incontinence? These are all common symptoms of pelvic organ prolapse (POP). Unfortunately, 2-48% of women may experience symptoms of POP.
Pelvic Floor Rehabilitation Treatment Options
There are treatment options such as pelvic floor rehabilitation through physical therapy techniques including lifestyle modifications such as managing intraabdominal pressure, promoting healthy bowel/bladder habits, as well as physical therapy, manual therapy, and strengthening exercises to decrease pelvic heaviness.
- Details
- Written by: Staff
- 18403 Views

What's the Connection Bewteen Eating Disorders and Pelvic Floor Dysfunction?
Read on for some answers.
Eating disorders are unfortunately common, with at least 9% of people worldwide suffering from an eating disorder. This translates to 28.8 million Americans will have an eating disorder in their lifetime. There are different types of eating disorders (ED) including anorexia nervosa, bulimia nervosa, and binge eating disorder. Other than the typical psychological and social implications that these eating disorders may cause, they also can affect our pelvic health and lead to pelvic floor dysfunction. It can lead to incontinence (either urine or feces), prolapse, increased urinary urge, pelvic pain (possibly associated with polycystic ovarian syndrome or PCOS), constipation, and sexual dysfunction.
- Details
- Written by: Staff
- 5777 Views
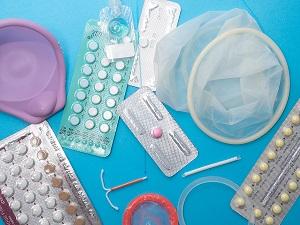
Contraceptives and Sexual Function Considered
As pelvic floor physical therapists, we work with a lot of women who have some type of female sexual dysfunction, whether it may be pain with initial penetration, pain with deep thrusting/deep penetration, pain with orgasms, or decreased sexual arousal, desire, libido. Unfortunately, about 30-50% of women may suffer from these symptoms.
We often see women with sexual impairments have the following conditions/scenarios:
- Postpartum (regardless of delivery)
- Vaginismus (involuntary spasms of the pelvic floor muscles)
- Post-menopausal
- Vulvodynia
- Skin inflammatory conditions such as lichen sclerosus
- Details
- Written by: Kasia Gondek, PT, DPT, CSCS
- 3999 Views

SMART Pelvic Health Goals
As we enter 2022, the new year marks a time of both reflection on the previous year and forward-thinking and planning for the year ahead. That’s why the beginning of the year is a great time to reset your pelvic health goals! Here at Femina Physical Therapy, we like to use the S.M.A.R.T. goal setting with frequent review of progress toward these goals. S.M.A.R.T. goals offer a simple and proven method of creating and evaluating goals that are reachable, specific and achievable. The S.M.A.R.T. acronym stands for:
- Specific (simple, sensible, significant).
- Measurable (to help motivate and track your progress).
- Achievable (attainable).
- Relevant (reasonable, results-based, unique to you).
- Time-bound (time-based, time-limited).
When creating your list of pelvic health goals, keep in mind what is relevant and meaningful to you. Visualize what achieving your goals might look like, how will it feel, what will your reward to yourself be? It is important to keep these critical aspects in mind when creating goals in order to determine if they are reasonable, achievable, and meaningful! Plus, a reward for achieving our goals keeps us motivated to push through challenges and roadblocks along the way.
- Details
- Written by: Heather Jeffcoat, DPT
- 7973 Views

Are You Wondering "Can A Vaginal Birth Ruin Your Sex Life?"
Medically, the answer is a resounding ‘no’… but postpartum sex is still an understandable concern for most pregnant women, especially in a digital age where whispered rumors have given way to detailed stories of difficult birth experiences splashed across social media pages.
In the greater debate over vaginal birth vs. C-section, the real issue on the minds of many expectant mothers is often whether one mode of delivery is somehow better than the other. It’s a complex question; but a group of researchers in Ontario, Canada recently attempted to answer the ‘sex after baby’ part of it. What they found out surprised even them; and shed some important light on the bigger question as well.
Researchers Studying the Impact of Vaginal Childbirth versus Cesarean on Postpartum Sex Find...
- Details
- Written by: Heather Jeffcoat, DPT
- 4125 Views

First some facts about pelvic floor dysfunction:
- Nearly one in two women experience painful sex.
- One in three women suffers from urinary incontinence.
- 40% of all women and 50% of childbearing women have pelvic organ prolapse.
Because I’m a fan of scientific data, this isn’t the first time you’ve seen the truth by the numbers in this space.
Rarely, though, do I get to talk about a ‘study of many studies’ like the one published in Sexual Medicine Reviews.
- Details
- Written by: Staff
- 4604 Views

A Pelvic Floor PT Can Assist With Cervical Cancer and Recovery
Cervical cancer is the fourth most common cancer affecting women worldwide.
Luckily there are many wonderful treatments that can stop the cancer, either completely or from progressing further. However, the treatments do come with some unwanted side effects. But there is help and having a pelvic floor physical therapist added to your ervical cancer support team can truly guide you along the way.
Common Cervical Cancer Treatments
Some common treatments are pelvic external beam radiotherapy and/or brachytherapy, which unfortunately can adversely affect women’s sexual functioning and quality of life. Radiotherapy especially can cause vaginal stenosis, which is narrowing of the vaginal canal. This is due to radiation effects of collagen deposition, loss of elasticity in the vaginal tissue, and atrophic changes of the mucosa. Unfortunately, 88% of women after radiation will develop vaginal stenosis. As you can imagine, narrowing of the vaginal canal can impede women’s ability to tolerate penetrative sexual intercourse or gynecologic exams, for example.
- Details
- Written by: Staff
- 6779 Views

Restless Legs Syndrome (or RLS)
Restless legs syndrome (or RLS) is a condition where there are uncontrollable urges to move limbs (mostly in the legs, but sometimes in the arms) that follows a circadian pattern, namely evenings/overnight when resting.
The urges usually come with unpleasant sensations such as tingling, burning, itching, or otherwise pain. Usually, it can be alleviated by movement, but as you can imagine, it can be debilitating and impair sleep, and thus the quality of life. It is common to experience mood swings, anxiety, and depression.
It is estimated that about 3.9-14.3% of the general population suffers from RLS. It is the most common movement disorder in pregnant women. There is either primary (idiopathic) RLS, or secondary (acquired) RLS due to pregnancy, renal pathologies, diabetes, hypertension, and other metabolic conditions. The two most common risk factors for RLS are iron deficiency and kidney disease.
- Details
- Written by: Staff
- 4480 Views

What is DRA?
Diastasis rectus abdominis (DRA, sometimes referred to as Diastasis Recti) is a distortion or thinning of the linea alba which is the midline of the abdomen that connects left and right rectus abdominis muscles together.
Although DRA can be found in both genders, it is more commonly found in females, and more common during pregnancy (66-100% of women have DRA during their third trimester) and can persist through their postpartum periods. About 33% of women continue to have a DRA a year postpartum. It can look like a gap in the midline, “doming” in the midline, or it can even appear as a “pooch,” in the lower abdomen.
Why Do We Care?
The abdominal muscles and linea alba assist in trunk movement, posture, lumbopelvic stability, breathing, and abdominal organ support. As you can imagine, it can affect those functions when a DRA is present. As movement specialists, we want to make sure you are engaging the muscles and tensing up the fascia of the linea alba appropriately to help prevent low back pain, pelvic girdle pain, and activity-related injuries.
- Details
- Written by: Staff
- 3321 Views

Safely Returning to Activity and Sport Postpartum
Postpartum Recovery Part 1
Most women get the clearance after their 6 week check-up for sex and exercise, YAY! But, really? How? What does that mean? There are no guidelines on how to return to activity in a safe, leak-free and pain-free manner.
Between 6 and 31% of postpartum women experience urinary incontinence. In addition, 66% of those who experience urinary incontinence during pregnancy and/or their first 3 months of postpartum continued to experience incontinence even at 12 years after birth! As you can see, it may be common, but it is certainly not normal!
- Details
- Written by: Staff
- 4173 Views
Breast Cancer Surgery and Physical Therapy - An Overview
There are an estimated 2 million breast cancer survivors in the United States and it is the most common form of cancer among women.2, 3 Following breast cancer surgery many patients experience neck, arm, and shoulder impairments. The most common complaints after surgery are restrictions in shoulder range of motion, pain, or a change in sensations of the arm and lymphedema.1
Common Side Effects After Breast Cancer Surgery
Restricted Arm Mobility
Women that experience restrictions in arm mobility following surgery report a lower quality of life and higher psychological distress.6 It is estimated that anywhere between 3.8–73% of women will have restricted arm motion following surgery.10
- Details
- Written by: Staff
- 6827 Views

What is IC or Interstitial cystitis?
IC is also known as bladder pain syndrome or painful bladder syndrome and is a debilitating condition that significantly affects the quality of life of patients living with it.
Many patients with IC have other overlapping pain conditions such as Dyspareunia (pain with intercourse). 88% of patients with IC had at least one symptoms of sexual dysfunction (lack of sexual interest, can’t relax and enjoy sex, difficulty becoming sexually aroused and difficulty reaching orgasm)1. Women with IC rated their sexual dysfunction as moderate to severe when compared to controls and reported increased pain with intercourse, decreased desire and decreased frequency of orgasm5,6.
- Details
- Written by: Heather Jeffcoat, DPT
- 14322 Views

Postoperative Care for Endometriosis Laparoscopic Procedures
Recovering from an endometriosis laparoscopic procedure requires proper care for a full and timely recovery. During this time there are some important steps to follow in order for everything to go smoothly. Here is a guide that will help ensure that you return to full health as soon as possible.
The First 48 Hours After Endometriosis Laparoscopic Surgery:
- Arrange for a partner, family member, or friend to drive you home and stay with you after your procedure. General anesthesia can cause nausea and vomiting. Having a bag or bin ready for the car ride home is a good idea.
- It can also be helpful to have a small pillow or cushion to put between your abdomen and seat belt for the ride home.
- Each surgery has unique guidelines specific to your case and what was done during surgery. Follow the guidance of your surgeon and pelvic health physical therapist. As this is a general guideline It is always a good idea to speak with your health care team prior to initiating any new exercise or protocol.
- Take it easy and rest for the first 24 hours.
- Finding a position of comfort: During the initial stage of recovery it is important to find a position that is comfortable to allow your body to rest and recover.









