
The Femina Physical Therapy Blog
Featuring original articles by our staff about current events and trends
With emphasis on vaginismus, pregnancy and postpartum best practices, treatments for incontinence, and other topics related to the health of your pelvic floor.
Featured From the Blog:
Introducing The Origin Fund - Helping Women in Need

Helping Women in Need With Our Community in Mind
The Origin Fund is dedicated to facilitating access to services that address a person’s physical, emotional and medical needs. Our focus is on individuals with pelvic health dysfunctions, and we are dedicated to improving the biopsychosocial aspects of each person as a whole. Through education, outreach and providing access to these services, we can support individuals on their journey to address their pain and dysfunction—linking patients to our network of referrals that provide these services.
Therapeutic Breast Massage in Lactation (TBML)

Therapeutic Breast Massage in Lactation Can Help Make Breastfeeding Less Painful
Breastfeeding is widely accepted as the normal standard for providing nutrition to newborns, however, many women who do not reach their breastfeeding goals. US national data stated that breast pain was a commonly reported reason for women weaning less than 1 month postpartum. Within that segment, 29% of women who participated in the study stated that “breastfeeding was too painful” to continue.
In the same study, 24% of women reported “breasts feel(ing) too full or engorged” as another reason to discontinue breastfeeding prior to 1 month postpartum.1 Currently, The American Academy of Pediatrics recommends exclusive breastfeeding of infants for the first six months of life. As physical therapists who treat patients with postpartum conditions, we are well positioned to make a big impact on patients with breastfeeding related pain and reduce barriers to continued breastfeeding!
Treating Bloating and Abdominal Distension: a Multi-Disciplinary Team

Why a Multi-Disciplinary Team is Best for Treating Bloating and Abdominal Distension
Bloating, abdominal distension, loose stools, constipation, abdominal or pelvic pain, fatigue, brain fog, weakness, nutritional deficiencies… these symptoms may be caused by a variety of gastrointestinal or pelvic conditions. If you are experiencing any of these symptoms, this article is a good place to start when deciding who to have on your care team, and what treatments can help!
- Details
- Written by: Staff
- 5670 Views

Recent studies have shown evidence vibration therapy is just as effective as massage in reducing muscle soreness after exercise and can also help increase range of motion.
Over the past few years, we’ve been using more vibration and percussive therapy products at the clinic, such as the Hypervolt gun, vibrating foam rollers, and vibrating massage balls. But what’s all the hype about?
Effect on Muscle Soreness
In a 2014 study by Imtiyaz et al., they found that a 5 minute session with a vibration device provided as much relief to muscle soreness as a 15 minute massage session over the same area, as compared to control groups who received neither after a bout of exercise.
- Details
- Written by: Staff
- 16858 Views
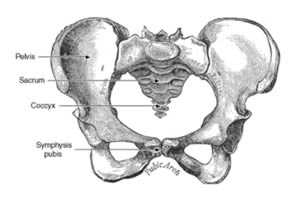
Sexual Dysfunction After Pelvic Fracture Can be Traumatic
A 2014 study by Harvey-Kelly et al. points to the fact that the long term consequences of this injury can include sexual dysfunction and pelvic pain for both males and females.
Pelvic fractures occur most commonly with a high-energy trauma. The most common ways people fracture their pelvis include motor vehicle (57%), pedestrians hit by car (18%), motorcycle crushes (9%), falls from a height (9%), and crush injuries (5%) (Harvey-Kelly, 2014).
Chronic Issues After Pelvic Fracture
Thanks to advancements in critical care medicine and acute trauma care, the mortality rate for those who have had a pelvic fracture has been reduced over the years. However, pelvic fracture survivors often report chronic issues including chronic pain, chronic pelvic pain, changes in gait, issues with bowel and bladder, and sexual dysfunction. This is because the muscles, bones, nerves, and blood vessels, are often all implicated in these injuries, and the pelvis contains the organs of the urinary, bowel, and sexual function systems. Therefore, the subsequent rehabilitation of all these systems is more complicated than, say, a fracture of your ulna or radius in your forearm.
- Details
- Written by: Staff
- 8318 Views

How do Histamines Affect Interstitial Cystitis (Painful Bladder Syndrome)?
Newly published research by Grundy et al. (2019) shows a more direct connection.
In this study published in the February 2021 issue of The American Journal of Physiology: Renal Physiology, Grundy et al. show correlation that histamines in the body lead to changes in the sensory nerves of the bladder, particularly hypersensitivity during bladder distension, or when the bladder is filling or full.
The study determined that certain sensory nerves in the bladder can become more sensitive when histamines are present. This activation occurs in the bladder membrane, the detrusor muscles, as well as the afferent nerves of the bladder.
- Details
- Written by: Staff
- 4617 Views

Simple Tips for Using Yoga for Sciatica Pain
Sciatic nerve pain can be uncomfortable and may affect your quality of life and your activities.
Flares in sciatic pain can be debilitating, and yoga for sciatica pain can help immensly. Often times the lower back and hips can contribute to sciatic pain. Try these yoga stretches for some relief.
This article is for informational purposes only and should not be considered medical advice. Please consult with your doctor or a physical therapist for an individualized session and exercises.
Here are some stretches you can do at home, at the gym, or at the park to keep your sciatic nerve pain at bay and enjoy your day pain-free.
- Details
- Written by: Staff
- 15943 Views

Dealing with too much tension? Try yoga to relieve your headache.
Tension headaches can be caused by tension in the jaw, face, neck, shoulders, and back.
Headaches caused by tight and restricted neck muscles can be helped by a seated neck release, which will stretch the scalene muscles on the neck. Sometimes headaches are caused by back pain that’s radiating up the spine, and yoga to relieve your headache may be the answer.
Try these simple poses to release the tension that may be giving you a headache.
- Details
- Written by: Staff
- 13780 Views

Lasers And My Vagina - Do They Really Belong Together?
A Breakdown of common Energy Based Devices Marketed for your Vagina
Risks and Possible Benefits
In the past decade, nonsurgical devices using radio-frequencies, lasers, and infrared light have been marketed as non-invasive treatments for “vaginal rejuvenation.” However, there has been conflicting opinion among the medical community as to what the lasers have evidence of treating. The rampant use of the lasers to treat conditions they have not been approved to treat has also caused the Food and Drug Administration to warn the public about these devices in 2018.
- Details
- Written by: Heather Jeffcoat, DPT
- 2200 Views
We wanted to share this article that we found published by the New England Journal of Medicine. We all have a lot of ongoing questions about the ongoing COVID-19 pandemic, and this is a great resource that answers nearly every question we’ve had regarding testing, vaccines and more.
Covid-19 Vaccine — Frequently Asked Questions

Image courtesy of NEJM
A collection of resources on Covid-19 vaccines, including frequently asked questions, continuing medical education, published research, and commentary.
CORONAVIRUS (COVID-19) VACCINE RESOURCES VACCINE FAQ
- Details
- Written by: Staff
- 15455 Views

Involving your partner in your pelvic floor therapy may improve your outcomes and your relationship.
Here are some ways you can involve your partner in your pelvic floor physical therapy:
Start Talking About Your Experience.
Both studies and clinical experience have shown that talking to your partner about your sexuality, pelvic floor issues, and sharing the progress you’re making in pelvic floor therapy can improve anxiety, reduce pain levels, and bring more intimacy to your relationship. As you transition to sex with your partner, sexual assertiveness will also help you find activities, angles, and positions that feel pleasurable, not painful to you and your partner.
- Details
- Written by: Staff
- 5310 Views

Stretching for health
Studies have foune that stretching improves joint range of motion (flexibility), decreases muscle tension, improves circulation, relieves muscle pain, prevents injury, and improves athletic performance (Nakaruma et al., 2015; Avela et al., 1999; Suzuki, 2005). Stretching the legs can allieviate low back, hip, and pelvic pain.
Here's a New Year's Stretching routine to get started. Please consult with your doctor or a rehabilitation therapist before beginning any exercise routines.
Tools Needed
- Yoga strap, dog leash, or robe strap
- A comfortable place to lay down (yoga mat or blanket)
- Details
- Written by: Staff
- 10510 Views

Here’s a simple foam roller routine to try for a happier pelvic floor this new year.
Foam rolling is a fantastic way to manage pelvic pain by keeping your tissues hydrated with increased blood flow, reducing trigger points in the muscles and fascia, and improving mobility and range of motion. Foam rolling has also been found to increase parasympathetic nervous system response (rest and digest) which is also helpful in chronic pain management (Beardsley, 2015).
I often tell my patients that the pelvic is not an isolated island, in fact it’s at the center of your body and deeply intertwined with many body functions including balance, movement, toileting, and sex. Go ahead and palpate your pelvic bones- you can feel that the muscles to the back, hip, and legs all attach to the pelvis. When there is dysfunction in these muscle groups, pelvic pain, pelvic mal-alignment, and tight pelvic floor muscles can be a result. By keeping these tissues healthy and mobile can help manage your pelvic pain.
- Details
- Written by: Staff
- 4839 Views

It’s that time of year when many of us are considering a diet change as a New Year’s Resolution. But with all of the wildly different diets out there, don’t let your new diet affect your pelvic floor health negatively.
Avoid Constipation
Constipation can contribute to pelvic pain, risk of prolapse, back pain, and pain with sex, among other issues.
As we’ve written about on this blog before, managing constipation is one of the cornerstones for maintaining pelvic health, especially if you suffer from pelvic pain, prolapse, or pain with sex. Constipation will lead to storage of old stool in the colon, which can contribute to pelvic, abdominal, and back pain. This added pressure can lead to pelvic floor tension and contribute to issues like pelvic pain and pelvic floor spasms. Last, but not least, constipation leads to straining on the toilet, which greatly increases your risk for issues like pelvic organ prolapse (read more about prolapse in this previous post).
- Details
- Written by: Staff
- 6540 Views

Communicating with your partner about your sexuality may reduce your pelvic pain and increase your sexual function.
A 2016 study by McNicoll et al. suggests that Sexual Assertiveness, or the ability to communicate openly to your partner about your sexual experience, may reduce the pain experienced with provoked vestibulodynia (PVD), increase sexual function, and encourage your partner to communicate you in ways that help boost your sexual health.
How Sexual Assertiveness May Reduce Your Pain
Pelvic pain and pain with sex may come from several different avenues, including vaginismus, vulvodynia, vestibulodynia, endometriosis, or tissue changes caused by menopause. The 2016 study by McNicoll et al. specifically worked with women with provoked vestibulodynia.
- Details
- Written by: Staff
- 9318 Views

What can a mother do to prepare her pelvic floor for pregnancy and childbirth?
First, you might be asking yourself “what is the pelvic floor”?
The pelvic floor is a group of muscles inside the pelvis that form a hammock from your pubic bone to your tailbone and from sit bone to sit bone on the sides. The function of these muscles are to stabilize your pelvis and spine, support your organs (bowel, bladder and uterus) and maintain continence. In pregnancy and childbirth, these muscles go through a lot of changes. The goal of this article is to try and achieve optimal pelvic floor function throughout pregnancy and after.
- Details
- Written by: Staff
- 4619 Views
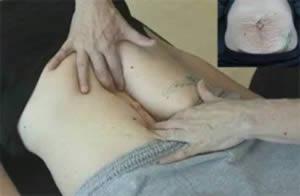
Mommy tummy aka diastasis recti abdominis (DRA) is a prevalent issue.
One in three American moms have DRA that persists greater than a year.
So what is a diastasis recti? It is the stretching of the linea alba, a connective tissue that runs down the midline of the abdomen and connects the abdominal muscles. The stretching happens during pregnancy in almost 100% of mothers to make room for a growing baby. Many of these moms are told this is a normal part of pregnancy, even by their healthcare providers.
DRA is not just about appearance, it is also connected to pelvic floor dysfunctions as well as pelvic and low back pain. In a study by Kari Bo et al., they found that mothers in the US with DRA were also more likely to have the following:
- Details
- Written by: Staff
- 5064 Views

Involuntary loss of urine during athletics is more common than you thought
Athletic incontinence is a type of stress incontinence that happens during an athletic event. Stress incontinence is an involuntary loss of urine due to a pressure or force like coughing, sneezing or jumping. When most people think of urinary incontinence they do not usually picture young athletes, however it is surprisingly common.
A study of young, elite athletes found 43% experienced urinary leakage while participating in their sport. The study also investigated which sports had higher incidences of incontinence:
- Details
- Written by: Staff
- 5657 Views

What studies say about returning to running as postpartum exercise
Most of the therapists in our office are moms, and we intimately understand wanting to get back to exercise after delivery. Caution should be taken when returning to running postpartum - we see this clinically and research also shows postpartum movement strategy changes that can increase your risk of injury.
A recent pilot study by Provenzano et al., 2019 compared the biomechanical changes of runners pre-pregnancy (or <14 weeks gestation and postpartum). They found at six weeks postpartum subjects had decreased trunk and pelvic rotation, decreased running speed, with increased step width and stance time compared to pre pregnancy measurements. They also found decreased motion in the hips with increased motion at the knee as a compensation.









