
The Femina Physical Therapy Blog
Featuring original articles by our staff about current events and trends
With emphasis on vaginismus, pregnancy and postpartum best practices, treatments for incontinence, and other topics related to the health of your pelvic floor.
Featured From the Blog:
Introducing The Origin Fund - Helping Women in Need

Helping Women in Need With Our Community in Mind
The Origin Fund is dedicated to facilitating access to services that address a person’s physical, emotional and medical needs. Our focus is on individuals with pelvic health dysfunctions, and we are dedicated to improving the biopsychosocial aspects of each person as a whole. Through education, outreach and providing access to these services, we can support individuals on their journey to address their pain and dysfunction—linking patients to our network of referrals that provide these services.
Therapeutic Breast Massage in Lactation (TBML)

Therapeutic Breast Massage in Lactation Can Help Make Breastfeeding Less Painful
Breastfeeding is widely accepted as the normal standard for providing nutrition to newborns, however, many women who do not reach their breastfeeding goals. US national data stated that breast pain was a commonly reported reason for women weaning less than 1 month postpartum. Within that segment, 29% of women who participated in the study stated that “breastfeeding was too painful” to continue.
In the same study, 24% of women reported “breasts feel(ing) too full or engorged” as another reason to discontinue breastfeeding prior to 1 month postpartum.1 Currently, The American Academy of Pediatrics recommends exclusive breastfeeding of infants for the first six months of life. As physical therapists who treat patients with postpartum conditions, we are well positioned to make a big impact on patients with breastfeeding related pain and reduce barriers to continued breastfeeding!
Treating Bloating and Abdominal Distension: a Multi-Disciplinary Team

Why a Multi-Disciplinary Team is Best for Treating Bloating and Abdominal Distension
Bloating, abdominal distension, loose stools, constipation, abdominal or pelvic pain, fatigue, brain fog, weakness, nutritional deficiencies… these symptoms may be caused by a variety of gastrointestinal or pelvic conditions. If you are experiencing any of these symptoms, this article is a good place to start when deciding who to have on your care team, and what treatments can help!
- Details
- Written by: Staff
- 6503 Views

Mental Health and Sexual Pain: Sexual Dysfunction is Not “In Your Head”.
We have seen that experiencing sexual pain CAN affect your mental health, and pre-existing mental health conditions can amplify sexual dysfunction.
This article will review the research related to these, but in reading, know that we believe your pain is real and should be addressed from all relevant contributing factors.
A very large range, about 7-46% of Americans may experience painful sex. For some, it may be a one-time painful experience, and for others, it may be every single time. This can have a huge effect on mental health and overall quality of life.
- Details
- Written by: Staff
- 6203 Views

You may have heard that chronic stress takes a toll on your body. But did you know how chronic stress affects your sex life?
What is chronic stress?
Chronic psychosocial stress is defined as either a major life event that takes place over a long period of time (ie. death of a family member) or small stressors that are constant and often accumulate (ie. traffic, financial worries, work deadlines).1,2 A study by Allen Kanner, Ph.D, published in the National Library of Medicine, found that these small stressors can have more of a negative effect on health than the more severe but less common stressors.1
How does chronic stress inhibit sexual arousal?
- Details
- Written by: Staff
- 4306 Views

Are You Thinking of Returning to Running Postpartum?
There is not a magic time frame as each person recovers differently and the most important thing is to listen to your body.
For healthy uncomplicated pregnancies and deliveries the American College of Obstetricians and Gynecologists (ACOG) recommends women return to low-moderate intensity exercise at six weeks postpartum and eight weeks postpartum for cesarean.
After your OBGYN or midwife has cleared you to return to exercise, if you haven’t started with a Pelvic Floor Physical Therapist yet, now is a good time.
- Details
- Written by: Staff
- 4835 Views

November is Bladder Health Awareness Month.
At Fusion Wellness & Physical Therapy, we take pride in understanding and applying how your whole body affects your pelvic health. In this article, we explore the links between grip strength and urinary incontinence.
A study conducted at the Jeju National University measured grip strength in patients and found statistically significant differences in patients with incontinence, overactive bladder and nocturia4. They found these patients had a weaker grip strength (less than 18kg) using a hand dynamometer.
- Details
- Written by: Staff
- 5695 Views

Physical therapy can help women across their lifespan. This includes support with orthopedic considerations related to breastfeeding, as well as other breastfeeding care with clogged milked ducts and noninfectious mastitis.
Symptoms & Causes of Clogged Milk Ducts and Mastitis
Breastfeeding can be a joyous time for some, but unfortunately it can be painful for others. Clogged milk ducts can be extremely uncomfortable and painful. It often arises due to not being able to drain fully, causing a back-up of milk along the mammillary ducts. It can occur when feeding sessions are interrupted or skipped, as well as when mom is under stress. One may experience symptoms such as a painful lump in the breast tissue, pain during breastfeeding that subsides after, and/or decreased milk supply from the blockage. Sometimes if unresolved, it can lead to mastitis, or infection of the breast tissue. Monitor for symptoms such as fever, swelling of breast tissue, redness of breast tissue, and escalation of pain/breast tenderness. If you start to experience these aforementioned symptoms, give your doctor a call as soon as possible.
- Details
- Written by: Staff
- 4441 Views
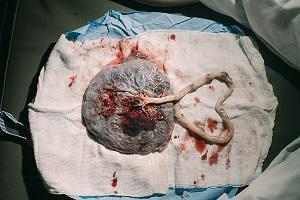
Third Stage of Childbirth: Delivery of the Placenta
You made it!
Now, at this point you have delivered your baby and your body’s hormones have shifted tremendously! You may feel overwhelming emotions of joy and exhaustion at the same time. Oxytocin, the bonding hormone, rises sharply to compensate for the drastic drop in estrogen and progesterone. You may find yourself shivering, and this is normal immediately post-giving birth and can last up to one hour.
Delivery of the Placenta
- Details
- Written by: Staff
- 9504 Views

Upright Labor Positions for the Second Stage of Labor
If you missed part 1 in the vaginal childbirth positioning series, go back and read it here.
Childbirth/labor is quite an experience, and it can be scary waiting for the unknown. Being prepared, knowing, and being familiar with different options and labor positions is the best way to approach childbirth to help decrease as much anxiety should surprises arise.
This article will go over specific labor positions that help progress labor, and prevent perineal trauma.
As mentioned in Part 1: Pre-Birth article, it’s important to keep changing labor positions to help progress, preferably in different upright labor positions. As a reminder, the first stage is all about increasing the pelvic inlet to help guide the baby through the mid pelvis and finally towards the pelvic outlet/vaginal canal.
- Details
- Written by: Staff
- 5237 Views

Positioning for the Pre-Birth Stage of Labor
What to Expect and What to Focus On:
If you have been pregnant for many months now, it is time to get ready for your upcoming birth! Similar to a marathon, we need to train for childbirth to prepare the muscles and body for the big event. For this reason, it is a good idea to start practicing being in different positions either with movement or holding a position for a long time. The pre-birth stage of labor involves contractions to dilate and open the cervix. Once the cervix is fully dilated, the second stage includes the passive and active phases of the baby crowning and coming out of the vaginal canal. The third stage involves the delivery of the placenta. We will go over how to best support our bodies throughout your childbirth journey.
Positioning for the Stages of Labor
Practicing and knowing different positions during this first stage can be helpful when pain may escalate. Upright positioning such as: walking, standing, rocking back and forth, kneeling over birthing ball, leaning against wall, holding onto partner are just some of the many, many positions that can be helpful.
- Details
- Written by: Staff
- 5546 Views

Postpartum Pelvic Health Recovery Should Start Day 1.
Here are some tips to help you get your postpartum pelvic health (and general health) back on track:
This article focuses on 5 key techniques you can use to improve postpartum pelvic health. It covers diaphragmatic breathing to activate core muscles and kickstart lymphatic drainage, pelvic floor muscle coordination, posture, and the benefits of a pelvic floor evaluation by a physical therapist to begin improving postpartum pelvic health on day 1. It also provides detailed instructions and references scientific studies to provide further research.
- Details
- Written by: Staff
- 5181 Views

Interstitial Cystitis, Multimodal Treatments, and How Pelvic Health Physical Therapy Helps IC
Interstitial cystitis (IC) also known as bladder pain syndrome or painful bladder syndrome, is a debilitating condition that significantly affects the quality of life of patients living with it.
The definition of IC from an international consensus is:
An unpleasant sensation (pain, pressure, discomfort) perceived to be related to the urinary bladder, associated with lower urinary tract symptoms of more than six weeks duration, in the absence of infection or other identifiable cause" (Hanno et al, 2009).
Interstitial cystitis affects 6-11% of women and 2–5% of men and increases with age from 1.7% under the age of 65 and up to 4.0% in women aged 80 years or older (Clemens et al., 2007 and Lifford et al., 2009). Patients that live with IC report that their quality of life is significantly impacted affecting their psychosocial, work-life, psychological well-being, personal relationships, and general health (Clemens et al., 2007). One important domain that is affected by IC is sexual function. Women with IC rated their sexual dysfunction as moderate to severe when compared to controls and reported increased pain with intercourse, decreased desire, and decreased frequency of orgasm (Peters et al., 2007 and Tincello et al., 2005).
- Details
- Written by: Staff
- 4342 Views

Whether you're asking for a friend or for yourself, it's an important question these days.
Practicing social distancing and wearing a mask can make it quite difficult to have intimate relationships.
Through the last year and half, we have learned more about COVID-19 and each and every day new data helps us better understand this virus and how to practice safe sex during COVID.
How is the virus transmitted?
The virus spreads through infected saliva, mucus, or respiratory particles entering the eyes, nose, or mouth. This means it can be transmitted through kissing and close contact. Studies have also detected the virus in feces and in sperm in those infected (Diangeng et al., 2020). It is unknown at this point if the virus can be spread through sperm or feces. Educating yourself can be the key to safe sex during COVID-19.
- Details
- Written by: Staff
- 15674 Views

Levator Ani Avulsion: Understand your pelvic anatomy to better understand your injury
The pelvic floor is a group of muscles positioned like a hammock along our saddle region.
The group of muscles attach from our pubic bone on the inside and then to our lateral pelvic walls with a bundle of collagen fibers called the levator arch, and attach to the ischial spines (the inside of the sit bones) and tailbone on the back side. During vaginal childbirth, the pubococcygeus muscle, a group of pelvic floor muscles, stretches 3.26 times more than its normal length to make room for the coming baby in the vaginal canal! As you can imagine, this may result in some perineal tearing and/or levator ani avulsion.
- Details
- Written by: Staff
- 8115 Views

A recent study connects anxiety, urinary incontinence and depression in women
What is urinary incontinence?
Urinary incontinence refers to the loss of urine, out of your control. There is actually more than one kind of urinary incontinence: the two most common types of urinary incontinence that affect women are stress incontinence and urge incontinence (also called overactive bladder, or OAB).
- Stress Incontinence: urine leaking with physical activity - sneezing, coughing, laughing, lifting, pushing/pulling, jumping.
- Urge Incontinence: urine leakage that is coupled with urgency to go- leaking while you’re in line for the toilet, leaking/urgency when you’re parking your car in the driveway, putting the key in the door, fumbling with your pants, etc.
- Mixed UI: a combination of stress and urge symptoms
- Details
- Written by: Staff
- 15666 Views

Pregnancy, labor, and delivery greatly affect the pelvic floor muscles, and our birth prep services using pelvic floor therapy can bring you confidence, strength, and flexibility.
What are the pelvic floor muscles?
The pelvic floor muscles are a group of muscles inside the pelvis that form a hammock connecting the pubic bone to the tailbone. Both men and women have pelvic floor muscles. These muscles play an important part in stabilizing the pelvis and spine, supporting your organs (bowel, bladder and uterus) and toileting.
The Pelvic Floor and Pregnancy
During pregnancy the pelvic floor muscles are working overtime trying to stabilize and support the growing body of the mother and child. Read our previous blog post about preparing the pelvic floor for childbirth. During a vaginal childbirth, these muscles will utilize their strength and flexibility to help the baby be birthed. Whether or not the baby is born via C-Section or vaginally, the pelvic floor is involved, and this is where our birth prep services come into play.
- Details
- Written by: Staff
- 5152 Views

A healthy lifestyle includes getting back to exercise postpartum
Exercise has shown to be beneficial in all stages of life, and the postpartum period is no exception.
Some of the benefits of postpartum exercise are:
- Strengthen and tone abdominal muscles
- Boosts energy
- May help prevent postpartum depression
- Promotes better sleep
- Relieves stress
- Can help you lose the extra weight that you may have gained during pregnancy
(ACOG, July 2019).
Even with all these benefits, research shows that most mothers stop participating in exercise programs which leads to increased weight gain and obesity (Minig et al., and O’Toole et al., 2003). There are many adjustments that have to be made when becoming a new mother and the information on the internet regarding postpartum exercise can be misguided and overwhelming. Let's break down what the literature says about guidelines for returning to exercise postpartum.
- Details
- Written by: Staff
- 9347 Views

The latest literature review conducted by Mazur-Bialy et al. (2020) shows the most modern methods of pelvic floor physical therapy that can help with urinary incontinence.
Here at Femina PT, we pride ourselves in keeping up with the current best practices and latest techniques. Here’s a breakdown of the latest techniques and how we utilize them at the clinic.
What is urinary incontinence?
Urinary incontinence refers to the involuntary loss of urine, which can range from a few drops (also called light bladder leakage) to complete loss that wets the floor. There is actually more than one kind of urinary incontinence: the two most common types of urinary incontinence that affect women are stress incontinence and urge incontinence (also called overactive bladder, or OAB).









