Learn All About Pelvic Organ Prolapse and the Role of Yoga in Recovery
Yoga can help manage pelvic organ prolapse, but there are also some poses, movements and breathing methods that could make the condition worse.

Featured From the Blog:

The Origin Fund is dedicated to facilitating access to services that address a person’s physical, emotional and medical needs. Our focus is on individuals with pelvic health dysfunctions, and we are dedicated to improving the biopsychosocial aspects of each person as a whole. Through education, outreach and providing access to these services, we can support individuals on their journey to address their pain and dysfunction—linking patients to our network of referrals that provide these services.

Breastfeeding is widely accepted as the normal standard for providing nutrition to newborns, however, many women who do not reach their breastfeeding goals. US national data stated that breast pain was a commonly reported reason for women weaning less than 1 month postpartum. Within that segment, 29% of women who participated in the study stated that “breastfeeding was too painful” to continue.
In the same study, 24% of women reported “breasts feel(ing) too full or engorged” as another reason to discontinue breastfeeding prior to 1 month postpartum.1 Currently, The American Academy of Pediatrics recommends exclusive breastfeeding of infants for the first six months of life. As physical therapists who treat patients with postpartum conditions, we are well positioned to make a big impact on patients with breastfeeding related pain and reduce barriers to continued breastfeeding!

Bloating, abdominal distension, loose stools, constipation, abdominal or pelvic pain, fatigue, brain fog, weakness, nutritional deficiencies… these symptoms may be caused by a variety of gastrointestinal or pelvic conditions. If you are experiencing any of these symptoms, this article is a good place to start when deciding who to have on your care team, and what treatments can help!
Constipation and pelvic floor disorders often go hand-in-hand for clients with hypertonic (tight) pelvic floor muscles and with associated symptoms like pelvic pain, pain with sex, and urge incontinence. So, let’s get your constipation in control!
If you think about what is housed inside of the pelvic bowl, three important systems have to co-exist and share a limited amount of space:
Read more: Manage Constipation...
User Rating: 5 / 5

With new year’s resolutions, a lot of us will be starting new workout routines to shape up. While exercise is a cornerstone of physical health, a little talked about side effect of increased athletic training, particularly for those with female anatomy, is urinary incontinence. A comprehensive literature review published March 2018 in International Urogynecology Journal found that female athletes have an increased the risk for urinary incontinence.
Read more: Exercise and Urinary...
User Rating: 5 / 5

Urinary incontinence is the loss of bladder control. Urinary incontinence affects up to 1 in 3 women. The two most common types of urinary incontinence that affect women are stress incontinence and urge incontinence (also called overactive bladder, or OAB). Incontinence affects twice as many women as men. This may be because pregnancy, childbirth, and menopause are contributing factors to urinary incontinence. Urinary incontinence should not be considered a normal part of aging, and it can be treated.
A new article published in September, 2018 by Lamerton, Torquati, & Brown found that being overweight (BMI 25-30) increased risk of urinary incontinence for young and middle aged by 35% and obesity (BMI ≥30) almost doubles the risk at 95%.
Read more: How Obesity Increases...

Two recently published articles, in the International Urogynecology Journal and in Neurourology and Urodynamics talk about the positive outcomes of treatment with trained pelvic floor therapists. Today is a basic rundown of what kinds of credentials, training, and skills a pelvic floor physical therapist has to offer you.
Pelvic floor therapists are often physical therapists (PT), a discipline that requires academically rigorous coursework and covers topics from anatomy and kinesiology, to neuroscience, and the evaluation, treatment, and management of common diagnoses. They are also trained in a medical system, and are aware of "red flags" in signs and symptoms that patients may present with. These "red flags" will typically require additional medical referral to rule in or out (i.e. suspected masses, infection, etc).
You will often find a jumble of letters after your pelvic floor therapist’s name. Here is a breakdown of what those letters mean:
PT, MPT, MSPT, or DPT: These letters represent the degree that your pelvic floor physical therapist earned. For many years, physical therapists earned a bachelor's degree prior to becoming licensed. Later, schools transitioned to master's degree programs. The letters MPT or MSPT indicates a master's degree in physical therapy. Most programs today now train therapists for a DPT degree, which stands for doctorate of physical therapy.
Read more: Why See a Pelvic Floor...
User Rating: 4.5 / 5

Menopause is a period of life transition for many of us. Today we will review what menopause is and how symptoms can negatively affect pelvic health, including bowel, bladder and sexual function.
Menopause is an important life transition for those with female anatomy, marking the end of the regular menstrual cycle and the transition to life beyond the reproductive period.
Babies born with female anatomy have a set number of eggs which are stored in their ovaries. The ovaries make the hormones estrogen and progesterone, which control monthly periods and ovulation. Menopause happens when ovaries no longer regularly release an egg every month and menstruation stops.
Read more: Menopause and Pelvic Health
User Rating: 5 / 5

According to the American College of Obstetricians and Gynecologists, more than half of those who have periods suffer from “dysmenorrhea” (pain associated with their cycles) 1-2 days each month.
There are two main causes of the pain associated with menstruation:
Read more: Painful Periods Treatment...
User Rating: 5 / 5

Tightly Wound has been released, watch it today and share it with your loved ones and anyone else who may need more education on vaginismus and pain with sex.
Tightly Wound is a 15-minute animated short by Shelby Hadden. Our very own Heather Jeffcoat, DPT is one of the producers of film.
Read more: Watch Tightly Wound!
User Rating: 5 / 5

A modified Pilates program can be a fantastic way to improve the strength of the pelvic floor muscles. A 2018 study by Lausen et al. had clients attend weekly one-hour Pilates classes over the course of six weeks. These classes used a type of Modified Pilates which consisted of Pilates exercises which had been modified and led by a physical therapist to specifically target the pelvic floor for the management of urinary incontinence. Those who attended the Pilates classes reported less leakage, improved self-esteem, decreased social embarrassment and lower impact of incontinence. Some of the women also reported improvement in their personal relationships after attending the classes.
In another 2011 study by Phrompaet et al., researchers found Pilates to be an effective treatment for instability in the low back and pelvis, which is a common contributor to pelvic pain and pelvic floor dysfunction.
Read more: Pilates and the Pelvic Floor
User Rating: 5 / 5

Yoga can help manage pelvic organ prolapse, but there are also some poses, movements and breathing methods that could make the condition worse.
"Prolapse" refers to a descending or drooping of organs. Pelvic organ prolapse (POP) refers to the prolapse or drooping of any of the pelvic floor organs, including: the bladder, uterus, vagina, small bowel, or rectum. These organs are said to prolapse if they descend into or outside of the vaginal canal or anus.
Read our previous blog for more information on prolapse and how pelvic floor therapy can help.
Yoga has been found to help women with urinary incontinence, but will it help with prolapse?
Read more: Pelvic Organ Prolapse and...
User Rating: 5 / 5

Rectal prolapse and hemorrhoids can both cause irritation, discomfort, and pain in the anal region. However the causes and treatment can be different for both conditions.
Hemorrhoids are veins in the lower rectum that become swollen or stretched. They are similar to varicose veins in the lower legs. There are two types of hemorrhoids: internal and external.
Internal hemorrhoids are swollen veins inside the rectum. Sometimes these swollen veins begin to descend and come out through the anal sphincter.
External hemorrhoids: are swollen veins that can be seen and often felt under the skin outside around the anal sphincter. Usually they look like a small bulge and are the same color as the skin.
Read more: What is the Difference...
User Rating: 4.5 / 5

A study presented at the annual meeting of the American Urological Association this past May of 2018 shows that a 3-month yoga intervention can reduce the frequency of urinary incontinence (UI) in women aged 50 years or older.
In the randomized trial completed by Dr. Alison Huang, MD and colleagues, a 3 month yoga therapy program was conducted with a group of 56 ambulatory women aged 50 years or older. These women had previously reported daily leaks and were not using any other clinical UI treatments.
The yoga program consisted of classes twice a week and one session of home practice weekly for three months. The therapeutic yoga classes were based out of the BKS Iyengar style of yoga.
After the three month trial, researchers saw a 74% decrease in daily leakage reported by the women in the yoga class. The women reported no negative outcomes related to the yoga practice.
Read more: Yoga Reduces Urinary...
User Rating: 5 / 5
Do you feel a bulge or feel like you are sitting on a ball in the pelvic area? What should you do? Don’t freak out, there is help for you! Here are some things to get you started:
Not all prolapses are the same. They can vary based on which organ is descending and how far it has descended (grade).
Prolapse will be diagnosed based on which organ is descending:
Read more: Body Mechanics and Posture...
User Rating: 5 / 5
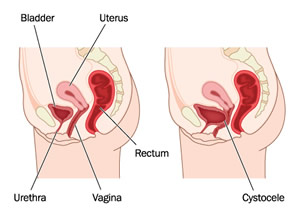
It’s Pelvic Organ Prolapse Awarenesss Month. Today we talk about something that’s often not talked about and lay out ways prolapse can be avoided and treated with proper pelvic floor physical therapy.
"Prolapse" refers to a descending or drooping of organs. Pelvic Organ Prolapse (POP) refers to the prolapse or drooping of any of the pelvic floor organs, including: the bladder, uterus, vagina, small bowel, or rectum. These organs are said to prolapse if they descend into or outside of the vaginal canal or anus.
Prolapse is sometimes given these specific names to describe which organ is descending:
Cystocele: The bladder falls backward into the front (anterior) vaginal wall
Urethrocele: A prolapse of the urethra (the tube that carries urine) into the vaginal wall
Uterine prolapse: prolapse of the uterus
Vaginal vault prolapse: prolapse of the vagina
Enterocele: Small bowel prolapse
Rectocele: the rectum falls forward into the back (or posterior) vaginal wall.
Read more: Treating Pelvic Organ...
User Rating: 5 / 5

On May 6, communities across the country including downtown LA gathered for the March for Moms to bring about changes to improve the health of mothers and birthing families in the United States. Femina Physical Therapy was there to join the national movement to address the maternal health crisis in our country. It was a wonderful day connecting with the community of concerned parents, community members, and health practitioners.
Together, we were able to call attention to issues affecting moms in Los Angeles.
Read more: Femina Physical Therapy and...
User Rating: 5 / 5

Last month the American College of Obstetricians and Gynecologists (ACOG) updated their position on postpartum care in the “fourth trimester” - the first 12 weeks after your baby is born. This is such a huge step for better healthcare and support for women after delivery. In other countries (France, Belgium, Northern Ireland and other European countries), postpartum physical therapy is a routine referral for women both in the hospital and for ongoing support when they are discharged.
The statement updates the previous recommendation of a 6 week visit, and instead supports a paradigm shift of postpartum care that not only adds contact with their Ob-Gyns within the first 3 weeks of delivery, but also address the need for ongoing care:
Read more: Redefining Postpartum Care...
User Rating: 5 / 5
After delivery via cesarean section, hysterectomy or other laparoscopic procedure, there will be an incision site that you will have to manage according to the directions of your doctors and nurses to keep the site from becoming infected. Although the incision site will close after about 2-3 weeks, scar tissue will continue to form. It is important to begin scar massage and desensitization techniques to help prevent scar tissue build up, puckering, and ongoing pain.
A trained physical therapist can perform soft tissue mobilization and other modalities such as cold laser over the scar site. As a part of your treatment, your therapist will teach you skills to manage the scars at home for the following benefits:
Read more: Scar Management and...
User Rating: 5 / 5
Page 11 of 13
Before I was referred to Heather Jeffcoat I was living in a nightmare. I had been married to my husband for three years and I was suffering from Vaginismus. That all changed when I visited my OBGYN and she said she knew of someone with a great success rate. To be honest I was hesitant at first because my first doctor had already told me that all I needed to do was order dilators from the internet and I should overcome my problem. She was wrong because I had followed the book on how to use the dilators with absolutely no advancements in my condition. However, that all changed when I went in for my first visit and Heather took the time to explain my condition and how we were going to work together to overcome it.
I remember leaving her office with a glimmer of hope that I could live a normal life. As my sessions continued I began to see immediate results. With only four sessions and a strict dedication to my home programs I was cured of Vaginismus. In the beginning of this process I was made aware that my health insurance company might not cover the costs, which was disappointing but today I can say one hundred percent that it was the best money I ever spent. Now thanks to Heather I am finally enjoying my life to the fullest with my husband. Thank you Heather, I can’t begin to tell you how much I appreciate all that you have done for me. I will never forget it. Those who are suffering from these types of conditions don’t be afraid because she makes you feel so comfortable and the end result is worth it. Good luck to you all and I hope you experience the success I have.
No one could tell me why I was having pain during sex--sharp pain, not just uncomfortable, pain. I was referred to Heather Jeffcoat after researching several different options. I had seen a specialist who told me physical therapy would not help and my only option was surgery. I really didn't want to go that route, so when we got a referral, I decided to try it--it can't hurt, I thought. I am so glad I did. She diagnosed the problem right away, which was a relief in itself.
To know why I was having pain eased my mind immensely. And to hear that she could fix it without surgery was another relief. She said she could fix the problem in 6 weeks. I think it was actually 4 for me. She was very methodical, and treated me as an intelligent human being capable of participating in my own recovery. I would absolutely recommend her to anyone. She did not try to prolong my session numbers, she worked hard to accommodate my schedule (and the fact that I had to bring a baby to sessions), and she was completely honest the entire time. It is so hard to find someone with these characteristics, much less a professional who is so good at what she does. She has my highest respect.
I went to Heather after the birth of my third child. It was lucky, really, that I was referred to her, because my doctor had referred me to a surgeon for a possible hysterectomy or pelvic wall rebuild. Thankfully, I went to Heather before undergoing either surgery, she was able to fix the problem. She has studied extensively in women's health--even written a book about it--and was able to diagnose my problem, suggest a course of treatment (6 weeks), and then follow through with said treatment. By the end, as she said, I was as good as gold. Boy, was it worth it! Though uncomfortable to talk about, much less write about, it is worth getting the word out there. If you have painful intercourse, especially after birth or other trauma, the treatment may be as simple as Physical Therapy (with Heather, of course). I highly recommend her.
Heather has affected my life in the MOST POSITIVE way and I am forever grateful. My husband refers to her as the "sex doctor" so you can only imagine how happy he is with my therapy outcome.
After the birth of my son I suffered from "Vaginismus", however, at the time I just thought I was broken. My "broken vagina" affected me physically but it was an emotional struggle as well. Many women in my life also suffered with pain from sex after their babies were born so I knew I wasn't alone. They told me they "just got used to it" but I couldn't see myself living that way.
Sex wasn't just painful, it was literally impossible - IT DIDNT FIT!
Heather has affected my life in the MOST POSITIVE way and I am forever grateful. My husband refers to her as the "sex doctor" so you can only imagine how happy he is with my therapy outcome.
After the birth of my son I suffered from "Vaginismus", however, at the time I just thought I was broken. My "broken vagina" affected me physically but it was an emotional struggle as well. Many women in my life also suffered with pain from sex after their babies were born so I knew I wasn't alone. They told me they "just got used to it" but I couldn't see myself living that way.
Sex wasn't just painful, it was literally impossible - IT DIDNT FIT!
I had tried Pelvic Floor Physical Therapy before (with another PT) and I had a really bad (painful) experience. A friend of mine and fellow patient, told me about Heather, Laureen and Femina PT (née Fusion Wellness & Physical Therapy) and I decided to try again. I am so happy I did! Femina PT have, literally, changed my life. I was able to do again things I couldn't do for over 10 years!! Their bedside manners are impeccable, their knowledge and understanding make me feel comfortable to recommend this place to anyone in pain. Specially if you have Endometriosis. 100% recommended!!

Like what you are seeing so far? Register for our mailing list and receive periodic updates via email, a 15% discount code for the "Sex Without Pain" ebook, and instant access to our Downloads area!